How to Take Your Blood Pressure at Home: An MD's Step-by-Step Guide
Dr. David Taylor, MD shows the step-by-step home blood pressure technique under the 2025 AHA/ACC ≥125/75 home threshold and the errors that inflate readings.
Updated
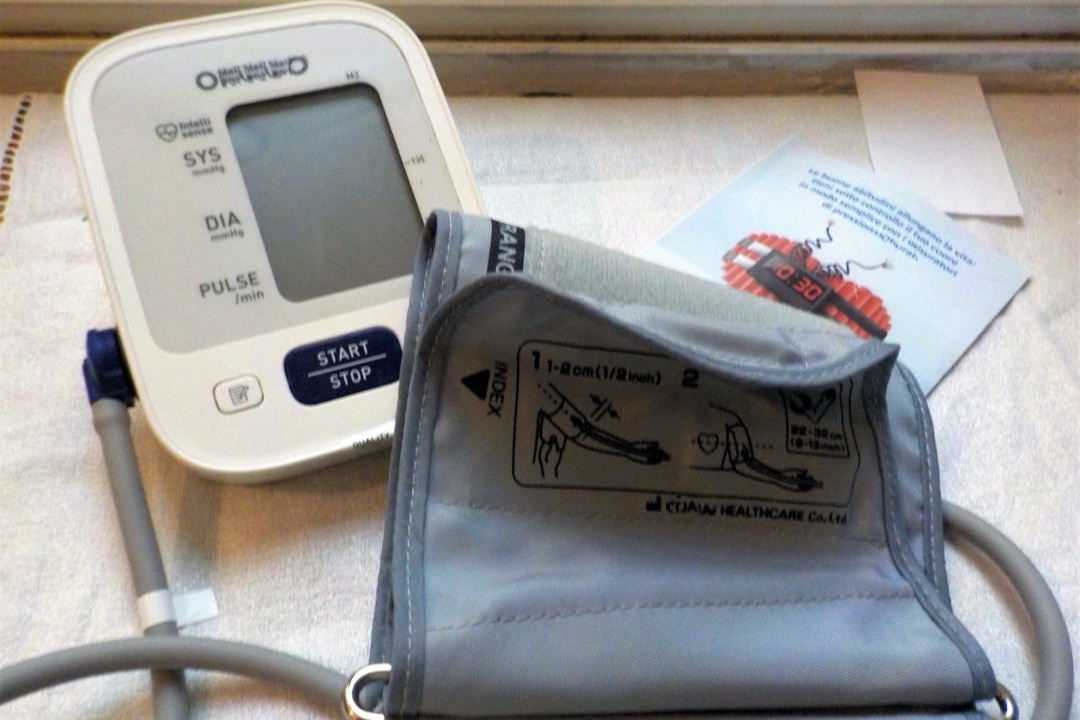
A patient came to see me last week because the pharmacy machine had given her a reading of 162/94 and she was convinced she needed emergency treatment. We retook her pressure in the office on a calibrated cuff, with her arm supported and her feet flat on the floor: 128/78. The pharmacy machine had not been wrong, exactly — it had measured what was in front of it. But what was in front of it was a woman who had jogged in from the parking lot, set her grocery bag on her lap, rested her arm on top of the bag (well above heart level), and let the machine inflate over her sweater sleeve. Three technique errors stacked, each adding a few millimeters of mercury. The number was real. The diagnosis it implied was not.
Home blood pressure monitoring is the most powerful diagnostic tool the average patient has access to — more powerful than a single office reading and, under the 2025 AHA/ACC hypertension guideline update, formally preferred for diagnosis and management. But it only works if you do it correctly. Studies estimate that more than 70 percent of self-measured readings in a research lab setting are wrong because of technique errors, and the cumulative effect of stacked errors can easily produce a 20 mmHg overestimate. This guide walks through everything I tell my patients, in the order I tell them — what device to buy, how to use it, when to measure, what the numbers mean, and what to do about them.
Why Home Blood Pressure Monitoring Matters More Than Office Readings
A single blood pressure reading taken in a doctor’s office is a snapshot. It captures one moment in a physiological signal that varies by 10 to 30 mmHg across the course of a normal day. Worse, the office setting itself distorts the signal. The most common pattern is white-coat hypertension — the patient whose blood pressure is genuinely normal at home but rises 20 to 30 mmHg in the medical setting because of anticipatory anxiety. Treating that patient as hypertensive based on office readings means prescribing medication for a condition they do not have and exposing them to the side effects of antihypertensive therapy without the benefit.
The mirror-image problem is masked hypertension — normal in the office, elevated everywhere else. These patients carry the full cardiovascular risk of hypertension but escape diagnosis because no one has ever measured them outside the clinic. Masked hypertension is more dangerous than white-coat hypertension precisely because it is invisible to conventional screening, and it is the single strongest argument for routine home monitoring in adults over 40.
The 2025 ACC/AHA hypertension guideline update reflects this reality. Home blood pressure monitoring (HBPM) is now the preferred method for confirming a diagnosis of hypertension and for titrating medications, with a single office reading reduced to a screening tool that triggers home measurement rather than a diagnostic endpoint in itself. The reproducibility benefit is straightforward: a 7-day protocol of twice-daily home readings produces 28 data points averaged across multiple physiological states, which estimates true blood pressure far more accurately than any one cuff inflation in a fluorescent-lit exam room.
What You Need: Choosing a Validated Home Monitor
The device matters. Not every monitor sold on the shelf has been clinically validated, and the difference between a validated device and a generic one is the difference between data your physician can act on and data that gets politely ignored.
What I tell my patients to look for: an automatic, oscillometric, upper-arm cuff monitor that has passed validation by the American Heart Association, the British and Irish Hypertension Society (BIHS), the European Society of Hypertension (ESH), or the STRIDE BP independent registry. Brands that consistently produce validated devices in this category include Omron, A&D Medical, and Welch Allyn, and our roundup of the best blood pressure monitors walks through the specific models that pass these standards and the cuff-size options each one offers.
Wrist monitors are a second-line choice. They can be accurate when used with strict positioning — wrist held at exact heart level, supported, motionless — but in real-world use that positioning discipline is rare, and the resulting readings can be 10 mmHg or more off the true value. I recommend wrist devices to patients whose upper-arm circumference exceeds the maximum cuff size on standard monitors, to patients with conditions that make upper-arm cuffing painful, and for travel use where packing a full upper-arm device is impractical. Our wrist blood pressure monitor guide covers the validated options and the positioning technique required to make them reliable.
Cuff sizing is the single most overlooked variable. Measure the circumference of your mid-upper arm — halfway between the shoulder and the elbow — and match it to the cuff size specifications on the device. A cuff that is too small for your arm artificially compresses the brachial artery and can elevate readings by 10 mmHg systolic and 8 mmHg diastolic. This is the most common reason a patient comes in with a “hypertension diagnosis” from a home cuff and turns out to be normotensive on a properly sized cuff. If your arm circumference exceeds 13 inches, you need a large cuff. Above 17 inches, you need extra-large. Do not assume the standard cuff that ships with the device fits you.
How to Take Your Blood Pressure at Home: Step-by-Step
This is the protocol I give every patient on a printed handout. It is not optional. The reason competitors’ articles average 600 words and ours runs to several thousand is that the details below are where the diagnostic accuracy lives.
- Prepare for 30 minutes before measuring. Empty your bladder. No caffeine, nicotine, alcohol, exercise, or large meals in the preceding 30 minutes. Each of these can independently raise blood pressure for an hour or more.
- Sit quietly for 5 minutes before the first reading. Feet flat on the floor — uncrossed. Back supported by the chair. Arm supported on a table. No phone, no television, no conversation. The 5-minute rest period is not a suggestion; it is part of the measurement.
- Use a bare arm. Cuff over a thin shirt sleeve is acceptable if rolling the sleeve up bunches it tightly above the cuff. Cuff over a thick sweater is not acceptable and will artifactually raise the reading.
- Position the cuff at heart level. The middle of the cuff should be at the level of the right atrium — roughly the level of the nipple on the chest. Rest your arm on a table or armrest at that height. Do not hold the arm up. An unsupported arm forces the muscles to contract isometrically, which raises blood pressure by 6 to 10 mmHg.
- Place the cuff correctly. The bottom edge of the cuff should be 1 inch (about 2.5 cm) above the antecubital crease — the bend of the elbow. The cuff’s artery marker should align with the inside of the upper arm where the brachial artery runs.
- Take two readings, one minute apart, and average them. Do not talk, move, or breathe deliberately during the measurement. Stay still and quiet. After the first reading completes, wait one full minute, then take the second. Average the two for the recorded value.
- Record both numbers, your pulse, and the time. Write down systolic, diastolic, heart rate, and the time of measurement. If your monitor has memory storage, that is convenient — but a paper log next to the device works equally well and forces you to engage with the numbers rather than glance at them.
When to Measure: Timing and Frequency
For diagnosing hypertension or evaluating a new medication, follow the AHA-recommended 7-day protocol: two readings in the morning, two readings in the evening, every day for 7 consecutive days. The average of all 28 readings — with the first day discarded, since it tends to be artificially elevated — is what your physician should use for diagnostic decisions.
The morning reading should be taken within 1 hour of waking, before breakfast, before caffeine, and before any antihypertensive medication. This captures your blood pressure at the medication trough — the period when drug levels are lowest and uncontrolled hypertension would manifest first. The evening reading should be taken before dinner and before any alcohol. Aim for the same approximate time each day; consistency matters more than precision.
Once your blood pressure is stable on treatment, you can step down to two or three days per week of morning and evening readings. Patients who measure their blood pressure 10 times a day, especially when they feel anxious, generate noise rather than information. The cuff inflation itself is mildly stressful; cycling through it repeatedly produces a self-reinforcing anxiety pattern that distorts the data and the patient’s relationship with their own physiology.
Common Errors That Inflate Readings (and Make You Miss the Real Number)
This is the section I wish more guides included, because every error below is something I see weekly in clinical practice. The numbers in parentheses are average effects from the published literature — your individual response may be larger.
- Too-small cuff (+10 systolic / +8 diastolic). The single most common error. Always measure your mid-upper-arm circumference and match it to the manufacturer’s size chart.
- Cuff over thick clothing (+5 / +3). A thin shirt is fine. A sweater is not.
- Unsupported arm held in the air (+6 / +10). Rest the arm on a table at heart level. Holding the arm up isometrically contracts shoulder and bicep muscles and elevates pressure.
- Crossed legs (+6 / +4). Both feet flat on the floor. Crossing legs at the knee compresses venous return and raises pressure.
- Talking during measurement (+10 / +8). Stay silent. The pressor effect of speaking is larger than most patients expect.
- Full bladder (+10 / +5). Use the bathroom before the 5-minute rest period.
- Caffeine in the prior hour (+5 to +10 systolic). Coffee within an hour of measurement reliably elevates readings.
- Recent exercise or stair-climbing (+5 to +20 systolic, depending on intensity). Wait 30 minutes after physical exertion.
- At-home anxiety about your own readings (variable, often +5 to +15). The home version of white coat — patients who fixate on a borderline reading and re-measure six times in a row generate a stress-induced artifact.
The cumulative effect matters. A patient who measures over a sweater, with an unsupported arm, with crossed legs, while talking to their spouse, after a cup of coffee, can easily produce a reading 25 mmHg above their true pressure. None of those errors is dramatic on its own. Stacked, they manufacture a hypertension diagnosis out of nothing.
Interpreting Your Numbers: Home vs Office Thresholds (2025 AHA/ACC Update)
This is where the 2025 guideline update matters and where most patients are working from outdated thresholds. Home blood pressure thresholds are lower than office thresholds because home readings, taken correctly and averaged, eliminate much of the white-coat inflation.
| Category | Office reading (mmHg) | Home reading average (mmHg) |
|---|---|---|
| Normal | < 120 / < 80 | < 120 / < 75 |
| Elevated | 120–129 / < 80 | 120–124 / < 75 |
| Stage 1 hypertension | 130–139 / 80–89 | 125–134 / 75–84 |
| Stage 2 hypertension | ≥ 140 / ≥ 90 | ≥ 135 / ≥ 85 |
| Hypertensive crisis | ≥ 180 / ≥ 120 | ≥ 180 / ≥ 120 |
The key number to remember: a home blood pressure average of 125/75 or above is no longer normal under the current guideline. Many patients are still working from the older 130/80 home threshold and are unknowingly in the stage 1 range.
When to call your doctor: a sustained home average of ≥135/85 over 7 days warrants a clinical conversation. You do not need to call urgently — these patterns develop over weeks to months — but it should not wait six months for your annual physical.
When to call 911: a single reading of ≥180/120 accompanied by chest pain, shortness of breath, severe headache, vision changes, weakness on one side, difficulty speaking, or confusion is a hypertensive emergency. Treat it as a stroke or cardiac event and go to the emergency room. A reading of ≥180/120 without symptoms is a hypertensive urgency — call your physician’s office the same day, but it is not an immediate 911 situation.
Special Situations Most Articles Miss
Atrial fibrillation. Oscillometric monitors — which is to say nearly all consumer home monitors — calculate blood pressure by detecting pressure oscillations in the cuff that correspond to arterial pulsations. In atrial fibrillation, the irregular and variable pulse strength produces erratic oscillation amplitudes, and the algorithms that translate those oscillations into a numeric reading become unreliable. Some monitors will flag an irregular heartbeat detected (IHB) icon; some will simply produce a number that varies wildly from reading to reading. If you have known atrial fibrillation, you need either a manual auscultation by a clinician for occasional confirmation or a device with a validated algorithm specifically for irregular rhythms. Patients who suspect they have AF — episodes of palpitations, irregular pulse on self-check — should consider a personal ECG monitor for rhythm documentation alongside their BP cuff, since a single-lead ECG strip is far more diagnostic for AF than oscillometric pulse irregularity flags.
Pregnancy. Home blood pressure monitoring during pregnancy is essential for preeclampsia surveillance, particularly after week 20. The threshold for concern in pregnancy is ≥140/90 — higher than the non-pregnant home threshold — because the maternal-fetal physiology of pregnancy involves intentional vasodilation and increased blood volume. Any reading at or above that threshold, especially if accompanied by headache, vision changes, right-upper-quadrant abdominal pain, or new edema, requires immediate evaluation. Pregnant patients should use an upper-arm validated cuff and confirm sizing fits as the arm circumference may change across pregnancy.
Diabetes. Patients with type 2 diabetes have a tighter blood pressure target — typically <130/80 sustained — because the cardiovascular and renal risk of hypertension is amplified in the diabetic population. Blood pressure and blood glucose are physiologically coupled: elevated glucose drives endothelial dysfunction that worsens hypertension, and several antihypertensive classes affect insulin sensitivity. Patients managing both conditions should pair their BP cuff with a glucose monitor and track the two together — patterns where BP rises during glycemic excursions are clinically meaningful.
Older adults and orthostatic blood pressure. Patients over 65, and any patient who reports lightheadedness on standing, should also measure standing blood pressure once a week. Take a seated reading using the standard protocol, then stand up and remeasure after 1 minute and again after 3 minutes. A drop of ≥20 mmHg systolic or ≥10 mmHg diastolic on standing defines orthostatic hypotension and is a fall risk that medication adjustments can usually mitigate. This is a common but underdiagnosed problem in older adults on multiple antihypertensives.
Cardiopulmonary patients. For patients with COPD, congestive heart failure, or sleep apnea, blood pressure context is improved by simultaneous oxygenation data. Episodes of nocturnal hypoxemia drive blood pressure elevations that won’t appear on daytime cuff readings, and a pulse oximeter used during symptomatic episodes provides the second variable that makes the BP data interpretable.
Fever and acute illness. Acute illness — fever, infection, dehydration — can transiently elevate or depress blood pressure and produce readings that are not representative of your baseline. If you are febrile, take your temperature with a validated digital thermometer and note the temperature alongside any blood pressure reading taken during the illness. Do not use illness-period readings to make medication decisions.
Medications and Substances That Affect Home Readings
This is the section I include because zero competing articles do, and it accounts for a meaningful fraction of the spurious “new hypertension” diagnoses I see. Many common medications and substances elevate blood pressure significantly, and patients are usually unaware.
- NSAIDs (ibuprofen, naproxen, diclofenac) raise blood pressure by 5 to 10 mmHg systolic through renal sodium retention. A patient who starts taking 600 mg of ibuprofen three times daily for joint pain can develop new “hypertension” within a week.
- Decongestants (pseudoephedrine, phenylephrine, oxymetazoline nasal spray) are direct vasoconstrictors and can raise systolic pressure by 10 to 15 mmHg. Cold-and-flu season is the most common reason for a sudden BP elevation in an otherwise stable patient.
- Stimulants: caffeine raises BP for about 60 minutes after intake; ADHD medications (methylphenidate, amphetamine salts) produce sustained elevations of 5 to 15 mmHg systolic; nicotine in any form is a potent acute pressor.
- Estrogen-containing oral contraceptives can elevate BP modestly in susceptible patients; this typically appears within the first 6 months of use.
- Licorice root (real licorice, not most candy “licorice” which is anise) blocks the enzyme that inactivates cortisol in the kidney and can produce dramatic hypertension at high intake.
- Energy drinks and high-caffeine pre-workout supplements combine caffeine with other stimulants and can produce acute hypertensive episodes, particularly in patients with underlying cardiovascular disease.
- Alcohol: chronic intake above moderate levels is a major and reversible cause of hypertension. Even acute alcohol intake the night before can elevate next-morning readings.
If your home readings climb unexpectedly, review every medication and supplement you have started in the prior month before assuming you have developed essential hypertension.
How to Log and Share Readings With Your Doctor
The goal is not to bring me 200 individual readings. The goal is to bring me averages.
A 7-day morning-and-evening log is the standard format. For each day, record morning average (two readings averaged) and evening average. At the end of 7 days, average all the morning readings and all the evening readings to produce two numbers per day, then average across days for an overall morning average and overall evening average. Discard day 1 from the analysis — first-day readings tend to be artificially elevated.
Paper logs work fine. Many monitors include built-in memory storage of the last 60 to 120 readings. Some patients prefer phone apps that sync via Bluetooth from the monitor and generate PDF reports — this category exists and is convenient, though no specific app has earned a clinical consensus recommendation. Bring whichever format you actually use. The format that gets used is the format that helps. For patients without a Bluetooth-linked monitor, our free blood pressure log does the averaging for you — type each reading, the row auto-classifies against current AHA categories, and the exported PDF includes the morning and evening averages I actually want to see.
What I do not need: 50 individual readings written in the margins of a notebook with no averaging. The data is there, but extracting an actionable signal from raw single readings during a 15-minute appointment is not practical. Bring the averages.
When Home Monitoring Isn’t Enough: Ambulatory BP Monitoring (ABPM)
Home blood pressure monitoring is the right tool for most diagnostic and management situations, but a small subset of patients benefit from ambulatory blood pressure monitoring — a 24-hour cuff that inflates automatically every 15 to 30 minutes during the day and every 30 to 60 minutes at night. ABPM is the gold standard for several specific questions:
- Nocturnal dipping. Healthy blood pressure drops 10 to 20 percent during sleep. Patients who fail to dip (“non-dippers”) or who reverse-dip (higher BP at night than during the day) carry significantly elevated cardiovascular risk that home daytime measurements cannot detect.
- Suspected white-coat or masked hypertension when home and office readings disagree dramatically.
- Suspected resistant hypertension in patients on three or more antihypertensive medications who are not at goal.
- Episodic symptoms suggesting paroxysmal hypertension or hypotension that might miss the timing of home readings.
Your physician will order ABPM when one of these questions is on the table. It does not replace home monitoring — it answers a question that home monitoring cannot — and most patients who get one ABPM study return to home monitoring as their day-to-day tool. Insurance coverage for ABPM has expanded under the 2025 guideline update for several specific indications.
The Bottom Line
Home blood pressure measurement is the most informative cardiovascular data you can generate yourself, and under the 2025 AHA/ACC guideline it is now the preferred basis for diagnosis and medication titration. The execution is what determines whether the data is useful. Use a validated upper-arm cuff sized to your actual arm — our home BP monitor guide reviews the models that meet the AHA, BIHS, ESH, and STRIDE BP standards. Follow the protocol: 30 minutes of preparation, 5 minutes of rest, bare arm, cuff at heart level, two readings averaged. Run a 7-day morning-and-evening cycle when you need diagnostic data. Remember that the home threshold under the current guideline is 125/75, not 130/80. And bring the averages — not the raw readings — to your physician. Done correctly, the cuff on your kitchen table is the most powerful diagnostic tool in your home.
Frequently Asked Questions
What is a normal home blood pressure reading?
How many times should I take my blood pressure at home?
Why is my home blood pressure higher than at the doctor's office?
Should I take my blood pressure before or after taking my medication?
Is a wrist blood pressure monitor accurate?
Related Articles
About the Reviewer

Dr. David Taylor, MD, PhD
Drexel University College of Medicine (MD), Indiana University School of Medicine (PhD)
Dr. David Taylor is a licensed physician and medical researcher who founded BestRatedDocs in 2016. With an MD from Drexel University and a PhD from Indiana University School of Medicine, he combines clinical expertise with a passion for health technology to provide evidence-based product recommendations. Dr. Taylor specializes in health informatics and regularly evaluates medical devices, diagnostic equipment, and therapeutic products to help healthcare professionals and patients make informed decisions.